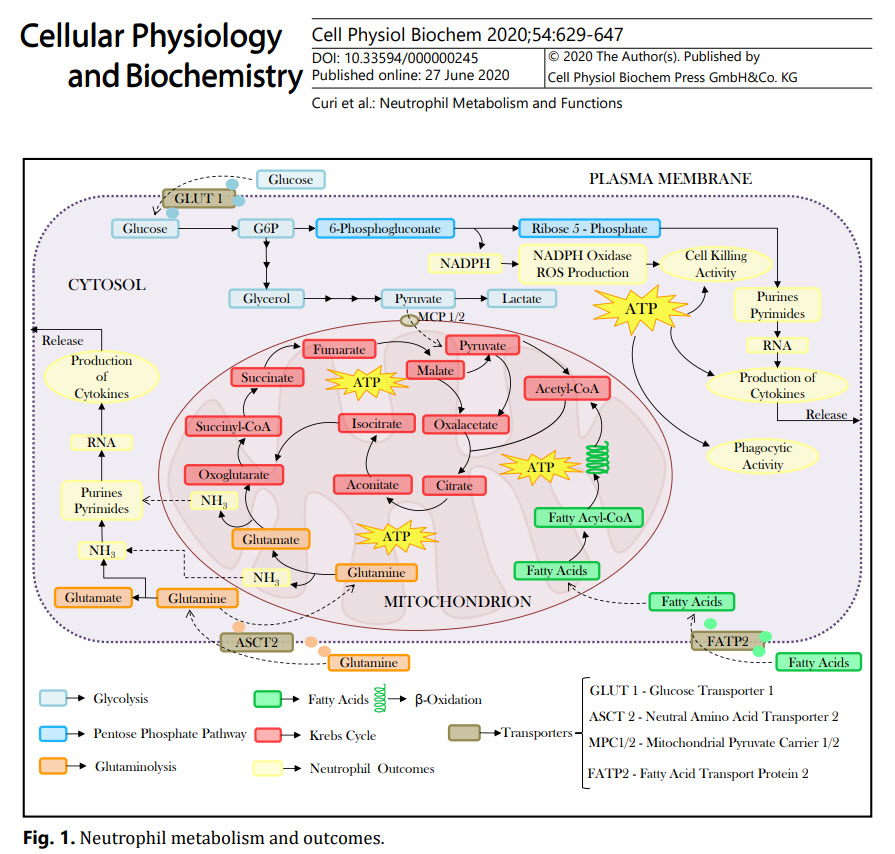
Neutrophils and Lactate
StudyLTCOVID.com
Thanks for visiting!
To translate this page, select your
language from the dropdown menu below:
From Exercise Physiology to ICU, Trauma and Emergency Medicine care,
studying and applying what has been learned about lactate and its metabolic effects and roles remains a popular topic.
If one approaches the topic from an interest in neutrophil dynamics and function,
one discovers that frequently applied concepts of anaerobic metabolism, and using lactate
levels as markers of physiologic stress, no longer offer a single or unified message.
And if tissue acidification leads to neutrophil activation (seems logical), is that activation associated with helpful or harmful effects ?
Not only are effects often found to be cell specific, but contrary or changing effects for
the same cell type are discovered when the cell changes tissue milieu. This, even when
settings like "tissue acidosis" to take one example, are not present and everything seems
normal or stable as it should be. Rather than limiting lactate to the role of a metabolic
waste product, its importance in cell signaling for example, clearly broadens its importance.
How this "broadened" view is modified by and in response to acute and chronic illness adds another level where previous concepts felt to be "rock solid," are found to no longer apply.
Even more true perhaps, in "long-term" COVID-19 (LTC) where beyond lactate, up to 57 different metabolites were found to be dysregulated.
Here are some articles that try to capture some of the current context for neutrophils and lactate interactions.
-----
Current Understanding on the Metabolism of Neutrophils
Emerging roles of lactate in acute and chronic inflammation
Extracellular Acidification Induces Human Neutrophil Activation
Lactate Is a Metabolic Mediator That Shapes Immune Cell Fate and Function
Late Neutrophil Priming Following a Single Session of High-intensity Interval Exercise
Role of Lactate in Inflammatory Processes__Friend or Foe
And here below, related to COVID-19, both acute and chronic:
Blood lactate concentration in COVID-19__a systematic literature review
The role of lactate in sepsis and COVID-19__Perspective from contracting skeletal muscle metabolism
The plasma metabolome of long COVID patients two years after infection
"The comparison of paired COVID-19/long COVID-19 samples revealed 53 metabolites that were statistically different. Compared to controls, 27 metabolites remained dysregulated even after two years."
"Lactic acid, lactate/pyruvate ratio, ornithine/citrulline ratio, and arginine were identified as the most relevant metabolites for distinguishing patients with more complicated long COVID evolution."
Lactate dehydrogenase contribution to symptom persistence in long COVID__A pooled analysis
The Critical Role of Cell Metabolism for Essential Neutrophil Functions
The graphic below, showing Neutrophil Metabolism and Outcomes is not offered to frighten nor impress. It does summarize what is known. It is from the article linked to just above.
It reminds that when it comes to lactate in health and disease, there is often proposed a simple answer, and it is wrong.
>>> Neutrophil Size Changes - a study in those with LTC and Normal Controls (NC)
>>> Introduction to Neutrophil cell membrane shape changes
>>> Our neutrophil shape change results in NC and LTC subjects
Can neutrophil-related damage be moderated by other than PBM?
Here's one example that is pertinent:
>>> Lots of related info about Colchicine
And another:
>>> Neutrophils and Multiple Sclerosis